TECHNOLOGY UPDATES IN OPHTHALMOLOGY
Rayner M-Flex 630F multifocal intraocular lens: functional results
FERNÁNDEZ-MARTÍNEZ C1, MARTÍNEZ-TOLDOS JJ2
Ophthalmology Service. General University
Hospital of Elche, Alicante, Spain.
1 Graduate in Medicine.
2 Ph.D. in Medicine.
ABSTRACT
Objective: To assess the functional result and degree of patient satisfaction after the implantation of the M-Flex 630 F +4 multifocal intraocular lens (Rayner Intraocular Lenses™. Ltd.).
Method: A prospective study was performed to assess far, near and intermediate visual acuity, presence of halos and degree of patient satisfaction 6 months after implanting the M-Flex 630 F lens with an additional power of +4. Twenty-six eyes were selected of a total number of 22 patients aged over 50 with cataracts as the only previous ocular pathology.
Results: The mean far visual acuity obtained was 20/25 (P<0.01). In the near distance, 16 of the 26 eyes (61.5%) exhibited visual acuity values equal to or above J3, and in 22 eyes (84.6%) the result was equal to or better than J5. In the middle distance, 18 of the 26 eyes (73%) exhibited visual acuity values equal to or above J3. Only 4 eyes exhibited presence of occasional halos. Of the 22 intervened patients, 21 (95.45%) referred that their visual satisfaction degree was «good» or «very good».
Conclusions: In the selected patients the refractive multifocal lens M-Flex 630 F +4 has achieved optimum functional results at all distances, exhibiting a low rate of undesired visual effects and providing a high degree of visual satisfaction.
Key words: Functional results, intraocular lens, visual acuity, cataracts, refractive surgery.
INTRODUCTION
An important challenge after the extraction of cataracts is to offer the patient an intraocular lens that will restore as much as possible the accommodative function of the lens. In order to continue improving the quality of life of patients, different multifocal lens designs have been developed, both refractive and diffractive. An important number of studies (1-11) have demonstrated that said multifocal lenses are not only capable of providing far visual acuity comparable to that of monofocal lenses but also achieve significantly improved near vision values. However, the literature also describes a significantly higher frequency of undesired luminosity events such as halos or flashes with monofocal lenses (2,12-14). In addition, several authors (1) have stated that some multifocal lenses do not provide good visual acuity for middle distances.
Even though it is true that progress is being made in the right direction with increasingly satisfactory functional results, there is still room for improvement.
In this study we present the results obtained after the implantation of the M-Flex 630F refractive multifocal intraocular lens (Rayner Intraocular Lenses. Ltd®) with additional power of +4. We analyzed far, near and middle distance visual acuity as well as the presence of halos and patient satisfaction degree.
MATERIAL AND METHODS
We designed a prospective, non-comparative study with the aim of assessing far visual acuity (6 meters), near visual acuity (33 cm) and middle distance visual acuity (70 cm), the presence of visual aberrations like halos and patient satisfaction (understood as comfort and independence of spectacles perceived by the patient in daily activities) (table 1). The variables used in the study were those collected 6 months after the intraocular lens implant.

The quantification of monocular visual acuity was made following the Snellen notation for all distances, adding Jaeger’s notation for close and middle distances. Visual satisfaction was sensed by asking the patient to define it as very good, good, average, poor or very poor. The patients were asked about the presence of halos in their vision. If the reply was affirmative, they were asked if the halos hindered their usual activities. The implanted lens was M-Flex 630F (Rayner Intraocular Lenses. Ltd®), manufactured with an acrylic and hydrophilic copolymer (Rayacryl®) and with an aspherical, refractive and multizone design (fig. 1). The additional power for near focus utilized in our study was +4. The lens power calculation was made with the SRK/T formula with the constant 118.5 (Iol Master. Zeiss®).
The data were analyzed with the statistical software SPSS version 13.0. The statistical significance was assessed with the t-student-fisher test for paired data, taking as significant any difference higher than P<0.05.
The patients were selected considering the following inclusion criteria (table 2): presence of cataracts without associated pseudoexfoliative syndrome, age over 50, emmetrope eye, absence of glaucoma, uveitis or retinal pathology history, far visual acuity prior to surgery under 20/40, previous keratometric cylinder under 1 dioptre, ability to understand and sign the informed consent.

All the interventions were performed by the same surgeon under topical anesthesia utilizing a 2.75 mm temporal corneal incision. After phakoemulsification, the cortex was irrigated and aspirated, implanting the intraocular lens in the capsular sac. At the end of the surgery all the patients received intrachamber antibiotic prophylaxis with cefuroxyme (1 mg in 0.1 ml of saline solution). In all cases the post-op treatment consisted in a fixed combination of tobramycin (3 mg/ml) and dexamethasone (1 mg/ml) (Tobradex®, Alcon-Cusí.) associated to ciprofloxacin 0.3% (Exocin®, Allergan) in descending dosage during 4 weeks. None of the cases exhibited events during or after surgery.
RESULTS
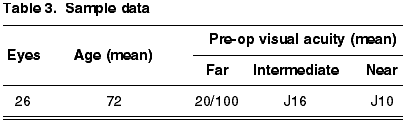
Twenty-six eyes were selected of 22 patients. As the objective of this study was to analyze the functional results obtained in each eye separately, it was decided to include four patients who were intervened in both eyes. The mean age of patients was 72 with a standard deviation of ±9 years. The mean pre-op visual acuity was 20/100 for long distances, J10 for near vision and J16 for middle distances (table 3).
The long distance results exhibited a highly significant improvement of the mean visual acuity 20/25 (P<0.01) (table 4). Of the 26 eyes of the study, 9 exhibited a visual acuity of 20/20. Other 12 cases had a visual acuity of 20/25 while 4 eyes exhibited a visual acuity of 20/30 and only one eye had a result of 20/40 (fig. 2).
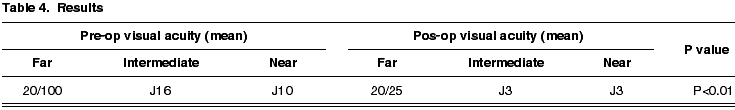
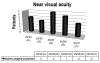
In the near distance, patients exhibited a mean visual acuity of 20/40 or J3 (P<0.01) (table 4). The results were distributed as follows: 9 eyes were between 20/25 and 20/30 (J1-J2), 7 eyes had 20/40 (J3), 6 cases had a visual acuity of 20/50 (J5) and 4 eyes gave a result of 20/70 (J7) (fig. 3). That is, 16 of the 26 analyzed eyes (61.5%) had near vision visual acuity values of J3 or better and 22 eyes (84.6%) exhibited a visual acuity of J5 or better.
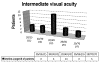
In what concerns the middle distance vision, the mean visual result was 20/40 or J3 (P<0.01) (table 4). In 8 cases a visual acuity between 20/25 and 20/30 (J1-J2) was recorded, while in 11 eyes the result was 20/40 (J3), 4 eyes exhibited a visual acuity of 20/50 (J5) and only 3 cases had a visual acuity of 20/70 (J7) or worse. In this case, 19 of the 26 eyes (73%) had visual acuity values of J3 or better J3 (fig. 4).
Only 4 eyes exhibited undesired visual effects in form of halos, described by patients as «occasional», mainly during the night and which did not interfere in any case with their usual activities.
In the visual satisfaction questionnaire, 17 patients rated their perceived comfort and visual independence for routine tasks as «very good», 4 as «good» and only 1 rated it as «average». No patient rated this variable as poor or very poor. In summary, 21 of 22 patients (95.45%) indicated they enjoy satisfactory eyesight free of dependence on spectacles for their routine activities.
DISCUSSION
Since inception, multifocal intraocular lenses have been the subject of numerous studies to provide evidence on their impact on the improvement of quality of life of patients.
In our study, 80.7% of intervened eyes exhibited a visual acuity of 20/25 or better in far vision and 61.5% exhibited visual acuity values of J3 or above in the near focus. As for the intermediate distance, 73% of cases exhibited results of J3 or better. Chiam PJ et al (9) obtained similar results with the ReZoom lens (Abbott Medical Optics®) in a study with 100 eyes, reporting a far binocular visual acuity of 20/25 or better in 88% of patients. They also reported visual acuity values of J3 or better in 74% of cases for the intermediate distance. In this study, 70% of patients stated they had an adequate independence of spectacles for their routine tasks. Finally, 30% of patients with ReZoom indicated the appearance of halo effects. Another prospective study with the multifocal refractive Array SA40N (AMO®) lens demonstrated that 67.3% of patients had near visual acuity values of J6 or better, while 56.6% has far visual acuity of 20/20 or better. In this study, 34% of patients exhibited halos and flashes, while 20% indicated visual dissatisfaction (15). The patients of our study exhibited occasional halos in 15.3% (4 eyes) and 95.45% indicated their satisfaction with their eyesight. Pineda-Fernández et al (16) reported in their study a visual acuity of J3 or better in 42.85% of patients of their study with the Array SA40N (AMO®) ands and a prevalence of halos of 18%. If we compare our results with those of said 3 studies, the refractive multifocal M-Flex 630F lens with the addition of +4 has achieved functional results similar to those published for the ReZoom lens and clearly superior to those published for the Array lens, exhibiting lower prevalence of halos and a high degree of patient satisfaction.
The good results obtained to date with multifocal lenses, specifically with the M-flex lens of our study, are good indicators of the improved quality of life of patients that can be expected with these optical designs. However, it must be taken into account that a careful selection of patients according to adequate criteria is probably the crucial step to ensure successful implantation of these lenses.
REFERENCES
-
Blaylock JF, Si Z, Vickers C. Visual and refractive status at different focal destances after implantation of the ReSTOR multifocal intraocular lens. J Cataract Refract Surg 2006; 32: 1464-1473.
-
Leyland M, Zinicola E. Multifocal versus monofocal intraocular lenses in cataract surgery: a systematic review. Ophtahlmology 2003; 110: 1789-98.
-
Javitt JC, Steinert RF. Cataract extraction with multifocal intraocular lens implantation: a multinational clinical trial evaluating clinical, functional, and quality-of-life aotcomes. Ophtalmology 2000; 107: 2040-48.
-
Kohnen T, Allen D, Boureau C, Dublineau P, Hartmann C, Mehdorn, Rozot P, Tassinari G. European multicenter study of the acrysoft ReSTOR apodezed difractive intraocular lense. Opthalmology 2006; 113: 578-584.
-
Blaylock JF, Si Z, Aitchison S, Prescott C. Visual function and change in quality of life after bilateral refractive lens exchange with the ReSTOR multifocal intraocular lense. J Refract Surg 2008; 24: 265-273.
-
Souza CE, Muccioli C, Soriano ES, et al. Visual performance of AcrySof ReSTOR apodized difractive IOL: a prospective comparative trial. Am J Ophthalmol 2006; 141: 827-32.
-
Mester U, Hunold W, Wesendahl T, Kaymak H. Functional outcomes after implantation of Tecnis ZM900 and Array SA40 multifocal intraocular lenses. J Cataract Rerfract Surg 2007; 33: 1033-40.
-
Hayashi K, Yoshida M, Hideyuki H. All-distance visual acuity and contrast visual acuity in eyes with a refractive multifocal intraocular lens with minimal added power. Ophthalmology 2009; 116: 401-8.
-
Chiam PJ, Chan JH, Haider SI, et al. Functional vision with bilateral ReZoom and ReSTOR intraocular lenses 6 months after cataract surgery. J Cataract Refract Surg 2007; 33: 2057-61.
-
Fernández-Vega L, Alfonso JF, Baamonde MB, Montés-Micó R. Symetric bilateral implantation of a distance-dominant diffractive bifocal lens. J Cataract Refract Surg 2007; 33: 1913-17.
-
Cillino S, Casuccio A, Di Pace F, Morreale R, Pillitteri F, Cillino G, Lodato G. One-year autcomes with new-generation multifocal intraocular lenses. Opthalmology 2008; 115: 1508-1516.
-
Dick HB, Krummenauer F, Schwenn O, et al. Objective and subjective evaluation of photic phenomena after monofocal and multifocal lens implantation. Ophthalmology 1999; 106: 1878-86.
-
Leyland MD, Langan L, Goolfee F, et al. Prospective randomised double-masked trial of bilateral multifocal, bifocal or monofocal intraocular lenses. Eye 2002; 16: 481-90.
-
Pieh S, Lackner B, Hanselmayer G, et al. Halo size under distance and near conditions in refractive multifocal intraocular lenses. Br J Ophthalmol 2001; 85: 816-21.
-
Sen HN, Sarikkola A-U, Uusitalo RJ, Laatikainen L. Quality of visión after AMO array multifocal intraocular lens implantation. J Cataract Refract Surg 2004; 30: 2483-93.
-
Pineda-Fernández, Jaramillo J, Celis V, Vargas J,DiStacio M, Galíndez A, Del Valle M. Refractive outcomes after bilateral multifocal intraocular lens implantation. J Cataract Refract Surg 2004; 30: 685-688.